Can the NHS modernise without going broke?
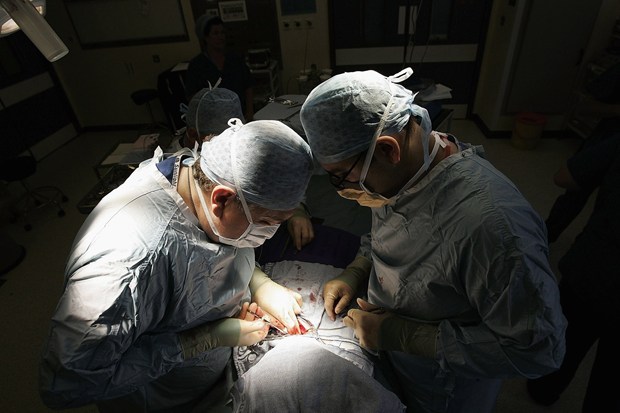
The NHS hopes its innovation testbeds, including hospitals in Birmingham and Solihull, will keep patients away from costly hospital stays and surgical procedures.
The NHS has a rotten reputation when it comes to technology. But insiders hope that could be about to change. A newly-launched testbed programme, bringing together patients, clinicians and technology companies, is aiming to tackle some of the health service’s most urgent problems. As an ageing population and funding uncertainties further stress its budget, the potential breakthrough couldn’t be more timely.
At Davos in January, NHS England CEO Simon Stevens announced seven innovation testbeds that will take a different approach to tackling the impending health crisis. The initiatives will address everything from long-term conditions such as diabetes and heart illness, to mental-health and old-age care.
In many ways the promise is worryingly familiar. In 2013, the parliamentary Public Accounts Committee called the national programme for IT – a project to digitise healthcare records – one of the “worst fiascos ever”, reporting the failure would cost more than £10 billion. A library of NHS-approved healthcare apps were revealed to be insecure, and last year the National Audit Office said a data-sharing system for GPs was over-budget, behind schedule and at the time only used by one clinic.

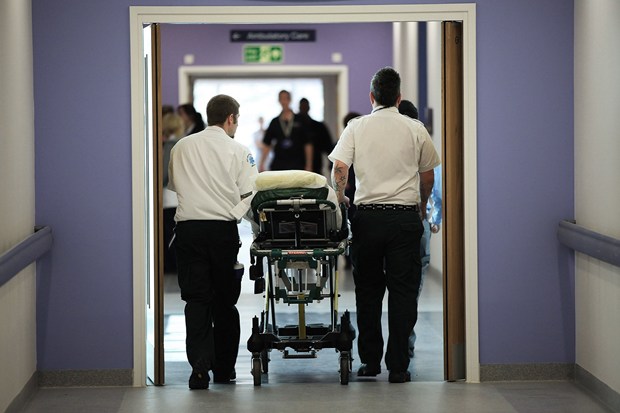
A&E admissions have risen by 25 per cent in the last ten years
Matt Cardy/Getty Images
The NHS can’t afford to not get technology right: the failures cost billions of pounds, and that doesn’t include the missed opportunity cost of using everything from big data to telehealth to improve treatment and keep people healthy out of hospitals. Hence the testbeds.
“What if you could reimagine healthcare either from the eyes of a startup or reimagine healthcare from non-traditional systems, such as a pharma?”
The testbeds evolved out of a five-year plan for the NHS, unveiled in 2014, that will try and work out how to balance budgets with caring for an increasingly elderly population. Two of the testbeds are focused on internet of things technology, with Surrey and Borders partnership NHS Foundation Trust using smart devices to help people with dementia stay at home longer and West of England’s Academic Health Science Network developing a diabetes digital coach.
The other five testbeds aren’t as prescriptive: in North East London and in Lancashire and Cumbria, testbeds are looking to support older people with dementia; Heywood, Middleton and Rochdale NHS is working with Google’s Verily on prediction and prevention techniques; Sheffield is looking to help people with diabetes, hypertension and other long-term condition treat themselves at home; and the Birmingham and Solihull project is developing tools for managing mental health.
All the projects are designed to help keep people out of expensive hospitals and clinics. A million patients visit the NHS every 36 hours and over the past decade the number of people attending A&E has risen 25 per cent. Alongside that, total hospital admissions have jumped 31 per cent, according to the NHS Confederation. That’s only expected to increase as demographics skew older, with the number of people 75 or older up by 89 per cent since the mid 1970s. As long term illnesses affect more people – as of 2013, there were 3.2 million people with diabetes – that’s expected to increase to four million within the decade. Budgets, meanwhile, are all but flat, and in 2013-2014 the NHS in ran a £471 million deficit.

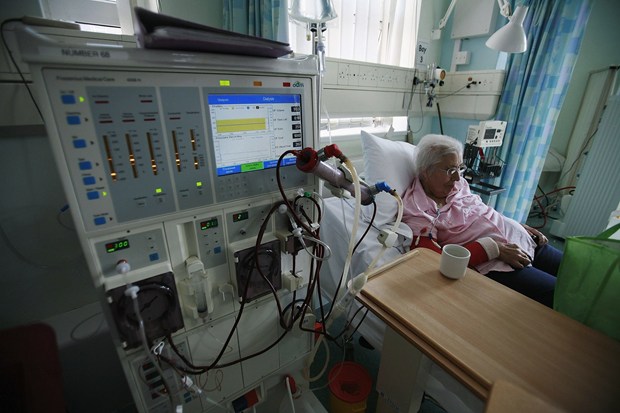
Digitisation of NHS records has struggled to get off the ground and is projected to cost over £10 billion
Photofusion/Universal Images Group via Getty Images
Mike Macdonnell is director of strategy at NHS England – which means part of his job is to help “modernise the health system without going broke”. It’s “partly fair” to criticise the NHS’s track record with technology, he says. “Certainly it’s not gone as well as we liked, and there have been some very well-publicised problems in the past.” But the testbeds will “try to do something different.”
How so? Macdonnell points to the idea of “combinatorial innovation” – a phrase he apologises for. “Increasingly, the nature of innovation is – to use a funny word – combinatorial.” Patents with a single name are on the decline, while “combination” patents that combine multiple organisations and ideas are on the rise. “This programme seeks to recognise that – putting together different technologies, entrepreneurs and innovators and then, importantly, pairing them in the real-world with NHS services.”
For example, in Rochdale, MSD, a division of German pharmaceutical giant Merck, is working with Verily (formerly Google Life Sciences) to figure out how to use predictive techniques to avoid people developing long-term conditions. And to do that, rather than simply put out a call for bids, Rochdale has the two companies getting the advice of patients and clinicians and one another. MSD’s director of healthcare services Junaid Bajwa admits the company doesn’t have the data science skills necessary for its project in Rochdale, so it’s teaming up with Verily. “What if you could reimagine healthcare either from the eyes of a startup or reimagine healthcare from non-traditional systems, such as a pharma?” he asks. “Who would you choose to work with?”
Steven Haigh, programme director for the Sheffield testbed, explains that rather than developing a product and taking it to market, or trialling an existing technology, the idea is to identify a problem that needs solving, and ask technology companies to work together to help come up with an answer. “We’re not just going to lob a lot of toys and goodies into the system and say: ‘Let’s make the best of it’, we’re going to do it completely the other way around,” says Haigh. “We want innovators [to] start talking to practitioners to say: ‘What are your biggest challenges and where are the biggest opportunities that technology could actually help’ – both [in terms of] helping keep patients independent and helping the services coordinate to learn in more effective ways.” In other words, the NHS – and that means the doctors, nurses and patients that make it up – will tell technology companies what they need, not the other way around.

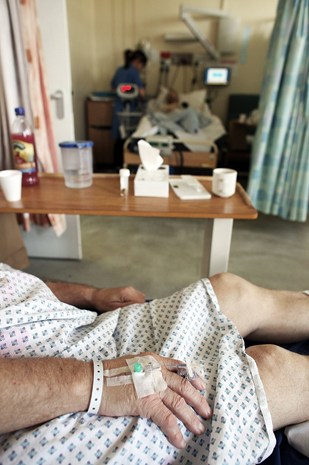
A greater focus on digital and patient-guided healthcare could relieve pressure on over-stretched hospitals
Photofusion/UIG via Getty Images
But what does that mean in practice? Meetings, workshops and surveys of clinicians and patients. Sheffield’s PEPPA (PErfect Patient PAthway) testbed is looking to help people with “complex needs”, defined as those with three or more long-term conditions. According to Haigh, that’s about 40,000 people in the Sheffield area alone. “We’re particularly interested in working with the population that has a mixture of physical and mental health needs,” says Haigh. “We’re interested in working with technology solutions that help people with their mental health well-being as much as their physical diseases such as diabetes, hypertension and so on.”
At the start of the testbed process the team cut down a list of 200 technology firms to 15 partners. “It’s not an exclusive list,” notes Haigh. “We just felt we needed to whittle it down to a reasonable number to work with.” The list ranges from companies making apps and devices, such as smart tech maker Kinesis, as well as “larger innovators” that will help with integration and the development of central platforms for patients and clinicians, including IBM, General Electric and Apple. Consultants from those companies are meeting frontline health workers and patients in a series of workshops to identify the “naughty, challenging problems” where technology can help.
For example, explains Haigh, community nurses spend a lot of time going into the homes of diabetic people to give them insulin. “We think some of the technologies that we could work with could actually help to the point where it’s the family or individual managing their own insulin injections. [The technology] tells us and reassures nurses that the patient actually has administered, so they don’t need to go in and check,” says Haigh. “If we could reduce the number of calls made by district nurses to patients that are insulin-dependent diabetics the productivity gains would be massive.”
The Sheffield project isn’t limited to diabetes. Staff will be working with practitioners over the next few months at a neighbourhood level to identify the problems in each local area – such as elderly people not getting enough help in home – before bringing those issues back to technology companies to develop a solution.
The Sheffield testbed will try to address the issue of elderly people not receiving enough medical attention in their own homes
Christopher Furlong/Getty Images
It’s hoped that putting NHS staff and patients, rather than technology firms, in control will keep the projects on-track, though it’s tough to see a series of workshops and surveys completely tipping the balance away from NHS executives and tech firms. A previous criticism raised by several of the clinicians and patients we spoke to of NHS innovation project was that they failed to include frontline staff and patients. “Projects like the NHS testbeds will succeed where they work closely with all stakeholders including, of course, patients, but also front-line staff who are aware of the intricacies involved in delivering the services in question,” says David Taylor, trustee from the Patients Association. “Where services have been designed with patients and front-line workers, they will be a better fit for the real needs of patients, and much more likely to be adopted and to work well.”
With that in mind, the testbeds have been tapping the experiences of so-called expert patients and patient groups. The former are patients who fully understand their condition, research alternative treatments and help others get better at living with the disease. In the West of England testbed, Sandra Tweddell, who has diabetes, fills that role. Tweddell is taking part in workshops and canvassing patient groups for their opinions about a diabetes digital coach that’s being trialled there.
Diagnosed with diabetes in 1961, she’s seen how technological advances have helped treatment evolve from guesswork to precision measuring at home. Her treatment is now largely self-managed, with only a few hours a year spent with healthcare professionals. As technology continues to improve, mistakes that lead to hospitalisation should also fall. “The aim is to keep your blood glucose level within a target range – a bit like walking a tightrope it’s very easy to fall off,” says Tweddell. If your glucose is too high, you risk blindness, limb amputation, kidney failure and more; if too low, you risk passing out. Some patients already have such tools, but Tweddell points out many can’t afford it, and they aren’t always supported by clinicians.
The number of people aged over 75 in the UK has increased by 89 per cent since the mid 1970s
Christopher Furlong/Getty Images
But there are other ways of making sure all patient voices are heard. In Sheffield, patients have the support of statutory body Healthwatch, a group that gathers feedback on the NHS and social care, using online and offline surveys to “seek voices that are seldom heard”. In September and October last year, the organisation took part in workshops to develop the testbed bid. According to manager Carrie McKenzie, the aim was to ensure the testbed was “reactive and responsive” and “not too prescriptive”, but also to ensure technologies are easy to use and don’t leave out less tech-savvy patients.
And some will be left out – a testbed project in the West of England, for example, is targeting just ten per cent take-up for its digital diabetes coach.
Even if some patients don’t end up using telehealth or accessing online platforms to update their own data, they could stand to benefit, according to Dr Phil Koczan. As part of UCLPartners, Koczan is advising the North London Care City testbed, which is looking for ways to better support older people facing dementia and other long-term conditions. “It’s not about having one or the other, it’s about bringing them together in parallel, so those who want to take advantage of technology will do so,” he says. “But we’re not making it any worse for those who don’t.” And by freeing up time, clinicians will be able to give more attention to those who can’t use technology.
Health care is about more than cutting costs, however. “It might mean, for some of the more vulnerable population, they get less social contact out of the healthcare system,” says Haigh. “While they may not see that as a problem at the moment, that may well be an unintended consequence if we’re not careful.”
Such issues will be taken into account when it comes to deciding if a project has been successful or not. The testbeds will be tracked by university researchers – for PEPPA, the University of Sheffield’s centre for health and related research has been commissioned to quantify success. Its baseline evaluation will then be used to score other technological interventions.
The myriad potential knock-on effects means that even if a testbed idea technically works, the NHS may ditch it – and Haigh says there’s no chance of a technology going forward if it doesn’t cut costs, regardless of other benefits. And that could make it hard to hold the attention of partner firms. “They’re coming in with no guarantee of a market share,” explains Haigh. “The risk is the innovators will not see where the opportunity is and disengage very quickly.” Getting that relationship right is key to success. But, Haigh continues, there’s more to success than future sales. “We’re giving them access to a sizeable population in which to test and develop their products, which they would otherwise not be able to access.”
And if those weren’t hurdles enough, there’s another challenge: the sheer scale of the NHS. What works in Sheffield or Rochdale will need to be translated to address specific problems in other areas of the country. That will be helped by the research tracking the testbeds, says Macdonnell. “We’re too slow to diffuse innovations, even when we get them working,” he says. “And I think that’s partly because we don’t have the right data to show that they are working. Real world, properly done evaluations with control groups are actually very few and far between. This programme will require them, and we’ll make sure we can show, with real robustness, that they’re doing better than existing practise.”
Despite evangelising technology, there’s a realisation that the real challenge lies in changing how doctors and nurses work, and how patients access health services. In this respect the testbeds aren’t about technology, they’re about finding a way to change how the NHS operates. “The technology is only part of the answer, and perhaps even the least important part of the answer,” says Macdonnell. “Changing the working practises around how patients access services and engage with services is at least as important.”
Hospital visits are projected to keep increasing each year, but budgets have flatlined
Christopher Furlong/Getty Images
While the NHS may have only just started running these testbeds, patients have been finding their own best practices and technology systems for years – and often paying for them out of pocket.
Andy Broomhead is the chairman of the Sheffield patient group for Diabetes UK – though he stresses he’s speaking in a personal capacity – and he’s already taken the care of his diabetes into his own hands. Broomhead gets about two hours of specialist time a year on the NHS, with no home visits, but has shifted to an insulin pump after a clinical trial and pays £48 every two weeks for a FreeStyle Libre sensor that means he doesn’t need to constantly stick a needle in his finger. Despite it making his life easier – and gathering more data for his self-management – it’s not paid for by the NHS.
“I think the pressure to manage finances in the short term may be a hindrance to allowing people to utilise technology for long-term benefit,” Broomhead argues. “For example, better glucose control over a period of five to ten years can help people reduce their risk of diabetes-related complications. But you don’t realise that benefit in the short term, so it may be harder for technology to be used or funded.”
“I think technology is used well in areas that can afford to provide it, but as those decisions are made at a [trust commissioning] level, funding and uptake is different across parts of the country,” he says. “I feel lucky to have access to a pump and I feel like it makes a huge difference to my life. I’m not sure there’s a huge level of technological innovation in my care per se, but I think what I have access to is a great benefit to me. I think, I hope, that my treatment will evolve over time as technology becomes better suited to solving the problems associated with living with diabetes.”
This is a long game. The testbeds will run for years rather than the usual weeks or months – and despite the optimism, uncertainties remain. The companies involved will have to wait years for revenue and there’s no guarantee that political interest will allow the projects to reach fruition. But for the NHS the challenge never changes: can the health service modernise without going broke?
WIRED Health 2016 will take place on 29 April in London. From helping humans live longer and hacking our performance, to repairing the body and understanding the brain, WIRED Health will hear from the innovators transforming this critical sector.
Now in its third year, tickets are still available for this incredibly popular one-day event. Discounts are available for NHS and government employees and for people working for health sector startups.